This is part IV in my mini-series on the role of dopamine in anorexia nervosa. In part I, I did a a little introduction on dopamine and dopamine signalling in the brain. In part II, I discussed preclinical studies using animal models to study the role of dopamine in AN. Finally, in part III, I talked about clinical studies using patients with AN to assess dopamine function. In this final post, I’ll review the evidence for using drugs that modulate the dopamine system in order to treat anorexia nervosa.
It is going to be short, because there’s really not that much evidence that any pharmacological agents help in treating anorexia nervosa. To quote the authors of this review study,
No single psychological intervention has shown clear superiority in treating adults with AN.
Most importantly,
… the first line of treatment for underweight patients with AN should be refeeding and weight restoration. This could be accomplished in a structured eating disorders treatment program without the use of medication (Barbarich et al., 2003).
However, in the last two posts, I provided some evidence suggesting that dopamine systems are affected in anorexia nervosa. If one of the problems in anorexia nervosa is increased dopaminergic receptor activity or increased dopaminergic signalling, one way to augment that might be through the use of antipsychotics, which work, in part, by blocking dopamine receptors.
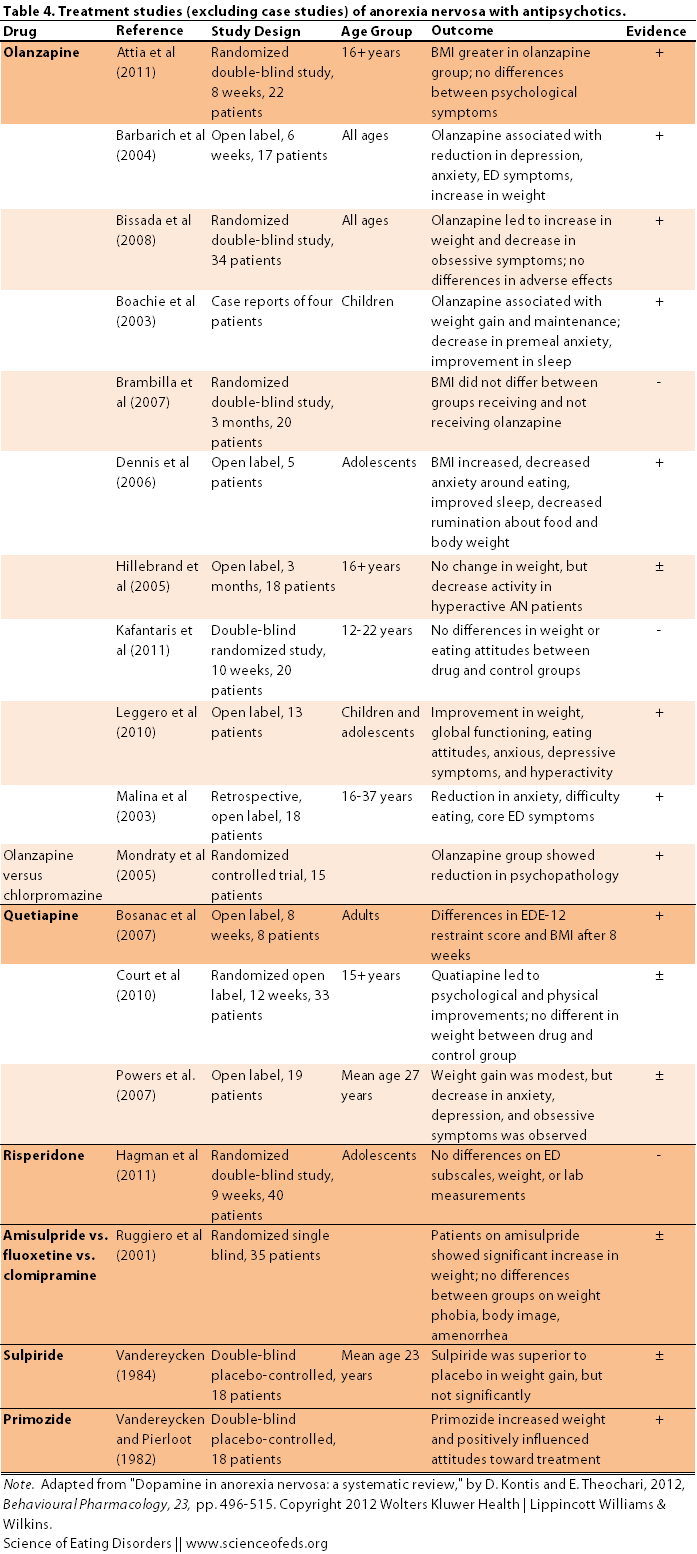
One antipsychotic drug that has been receiving a lot of attention with respect to anorexia nervosa is olanzapine, also known on the market as zyprexa. In the table below I summarized some of the studies on antipsychotics in anorexia nervosa, including olanzapine. I adopted this table from Kontis & Theochari (2012), taking out most case studies (except for one).
As you can see, when it comes to anorexia nervosa, olanzapine has been, by far, the most studied antipsychotic.
Based on these studies, I think the evidence for olanzapine having some ability to decrease anxiety and eating disorders thoughts is promising. The studies are generally small, of course, and we’d need much bigger studies to really confirm that olanzapine can help decrease anxiety and eating disorder psychopathology, without all of the terrible side-effects that antipsychotic drugs often have (and there are a lot of them).
I doubt there will ever be a drug that will “cure” AN. I don’t think these drugs are meant to do that–they shouldn’t be meant to do that, anyway. Maybe sometime in the distant future, but certainly not any time soon.
Recovering from an eating disorder is really hard work, and no drug is going to cure anorexia nervosa. This is because anorexia nervosa is complex: it is not caused by over-active dopamine receptors, or an over-active serotonin system. It might be partly caused by those things, in some people, but, on the whole, the causes are complex and not well understood at this point. We do know, however, that both genes and environment play a role. Finding a drug that will “fix” all of these various problems without side-effects, well, I’m not sure that will happen any time soon, if ever.
But here is where I think drugs might be useful for some people: in ameliorating co-morbid conditions such as anxiety or depression. Antidepressants, for example, can do a good job of decreasing anxiety in some individuals, and decreasing that anxiety might enable individuals to eat more, for example, or, as in bulimia nervosa, decrease the frequency of bingeing and purging. These drugs will not cure eating disorder patients, but for some, they might facilitate recovery by helping individuals make necessary changes to their behaviours.
(And then, of course, there’s the question of whether the possible benefits of these drugs outweigh the risks.)
References
Kontis, D., & Theochari, E. (2012). Dopamine in anorexia nervosa Behavioural Pharmacology, 23 (5 and 6), 496-515 DOI: 10.1097/FBP.0b013e328357e115
I was given zyprexa at 16 for depression. It caused a 24-pound weight gain in just six weeks. I was a healthy weight and had no issues with my body or eating. I subsequently developed anorexia. I do not believe I ever would have had it if it were not for that medication. I only had weight/body image issues after having gained the weight and it completely changed my body. I find it to be a slap in the face that they now use it for treatment in anorexia. It almost killed me and took away seven years of my life trying to fight against it.
Hi Anon,
I’m really sorry to hear about your awful experiences with olanzapine. As far as I know, I don’t think olanzapine is being used to treat anorexia nervosa–these were just treatment studies to test if it is effective. I’m not sure it is used in a clinical setting, and if so, it is probably rare. But I’m not 100% sure.
Tetyana
Very timely post for me, as my nutritionist just a couple weeks ago mentioned this idea of treating AN with anti-psychotics – I think she specifically mentioned Haldol and that it was a study done in…uh, somewhere in Europe. She did say that it showed some benefit, but like you say here, she felt that it was probably more about ameliorating attenuating circumstances/disorders. She also assured me she was not recommending we try it mainly because, like you say, the side effects of these drugs can be horrible.
But it is sort of intriguing that a drug used for, say, schizophrenia could also help with an ED. It fascinates me to think about the underlying similarities among various forms of mental disorders. (Obviously EDs are not just mental disorders, but they certainly are in part.)
Even if these drugs aren’t “cures” or even strongly effective medications for EDs, it is at least good to know there are people doing these studies and trying to find ways to help patients. Much better than so many who just brush it off or don’t think of EDs as “real”.
Yeah, as much as the trials seem to be more positive than I’d expect, I’m just weary of anti-psychotics. The side-effects are scary.
I’m curious why you say that EDs are not “just” mental disorders? What do you mean by that?
Hi. Great article, I am writing a memoir on AN and I want to get as clued up on the neuroscience as possible. Can you recommend any resources?
Hi Tabitha,
What kind of resources are you looking for exactly? There is lots out there, but it may be too technical; I’m not aware of any very good non-technical resources covering the neuroscience of AN . You can check out Carrie Arnold’s book (Decoding Anorexia), but I have not read it so I can’t speak about whether it will have the info you are looking for or not.
Cheers,
Tetyana
(And sorry for taking forever to respond; I am just going through comments I forgot to respond to when things were super busy.)