Few people would claim to like the sound of chewing, lip smacking, or pen clicking. But while disliking these noises is commonplace, experiencing anxiety, panic and/or rage in response to them–a condition called misophonia (hatred of sound)–is not.
Well, truth be told, we don’t actually know how common it is: Searching “misophonia” in PubMed returns just 14 results. Seven were published in 2013/2014, and only three were published prior to 2010. (Searching “selective sensory sensitivity syndrome,” another name for “misophonia” wasn’t particularly fruitful either.)
Interestingly, the most recent paper on misophonia investigated the phenomenon in eating disorder patients. Timely, I thought, given that a few months ago someone had asked me about this very thing on Tumblr. At the time, I came up with nothing. Now I had something. So I posted it on the SEDs Tumblr. The response was almost immediate (click here to read some of the responses). To be honest, I was surprised: I had no idea so many people could relate.
So I thought, it would be important to blog about this paper, which describes ED patients’ experiences with misophonia. In the study, Hannah Kluckow and colleagues screened for misophonia in 15 consecutive patients who had been treated for an eating disorder. Three fulfilled Schröder et al.’s (2013) proposed diagnostic criteria for misophonia.
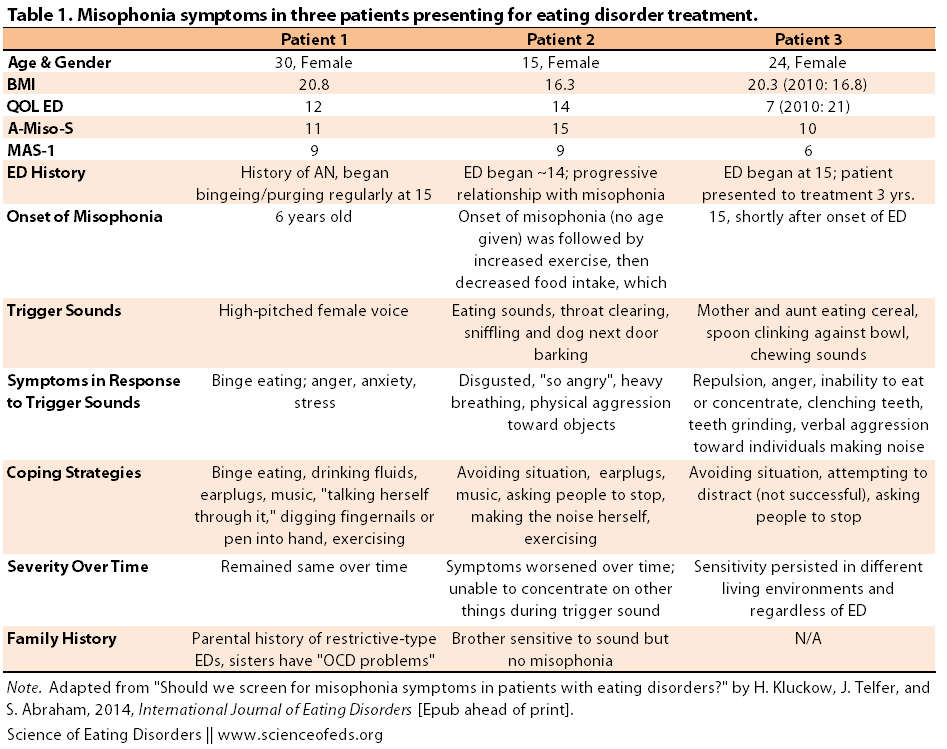
Kluckow et al. interviewed the patients about their symptoms and symptom history, and assessed their quality of life, misophonia symptoms, and severity of misophonia using questionnaires. I summarized the patients’ information in Table 1 below (click on table to enlarge):
WHAT CAN WE LEARN FROM THESE & OTHER CASES?
For one, it is clear that there is variability in the temporal relationships between ED onset and misophonia onset: one does not necessarily precede the other. In addition, there doesn’t appear to be a relationship between the severity of misophonia and the severity of the ED: severity of misophonia stayed the same or worsened for two patients whose ED symptoms improved.
For two patients, the primary triggers were sounds of chewing, eating, and crunching. I wondered if this might be related to the ED. Are chewing and eating noises common triggers for misophonia patients without an ED? As it turns out, they are.
In a case series of 11 subjects (4 males and 7 females, mean age: 36, age range: 19-65), all participants considered eating, chewing and crunching sounds to be among the worst triggers (Edelstein et al., 2013). Indeed, “eating/chewing/crunching” sounds were the only sounds that were considered a trigger by all participants of the study. (The paper, which is quite interesting, is also freely available online, and has been blogged about by fellow science/research bloggers.)
Several participants (in both studies) reported that they felt particularly bothered when the trigger noises originated from particular individuals. Though most of the participants were not bothered when they themselves were making those noises. Interesting, right?
WHAT ABOUT COMORBIDITIES?
In the Kluckow et al. study, all three patients had features of obsessive-compulsive personality disorder but none fulfilled the diagnostic criteria. In the Edelstein et al. study, only two of the eleven participants had OCPD traits. Conversely, Schröder et al. found that 52% of their sample (22/42 participants) had OCPD.
Schröder et al.:
This high comorbidity does raise the question of whether OCPD is a predisposing factor in the development of misophonia or a consequence of having misophonia. It has been reported previously that some individuals with impulsive aggressive problems develop OCPD symptoms in an attempt to compensate for an underlying problem with behavioural inhibition. This does not hold for our sample because in misophonia the impulsive aggression is only related to certain sounds.
They add:
From a phenomenological viewpoint, there appears to be an obsessional part, the focus and preoccupation on a particular sound, and an impulsive part, the urge to perform an aggressive action.
Most patients with OCPD do not have misophonia, but it appears that a substantial portion of patients with anorexia nervosa have OCPD. In a study by Strober et al. (2007), 36% of AN patients met the criteria for OCPD, and OCPD was three times more prevalent among relatives of AN patients than among relatives of healthy controls.
MISOPHONIA, OCPD, and EATING DISORDERS?
In their discussion Kluckow et al. suggest that misophonia, OCD (though I’d say obsessive-compulsive traits), and anorexia nervosa all share the same pathology and/or underlying causes:
It is suggested that misophonia and OCD may share related neurocircuitry with the dysregulation of serotonin and dopamine in the limbic system and basal ganglia. Inefficient dopamine and serotonin utilization can cause exaggerated aversive processing and compulsivity, which are common to misophonia and OCD. The clinical similarities between OCD and misophonia have been discussed in the literature, although they have been delineated as distinct patterns of symptoms.
And as I’ve blogged about before (here, here, here, and here, for starters), serotonin and dopamine systems are affected in AN and BN patients as well. So, maybe there’s a link there? If there is, we are still quite the ways from figuring it all out. After all, searching “eating disorder” in PubMed turns up over 30,000 hits, and we still don’t know all that much about eating disorders. “Misophonia,” as I mentioned earlier, only results in 14 hits.
FUTURE DIRECTIONS
Obviously, we need more research. It will be important to determine how prevalent misophonia is among ED patients. Is it more prevalent among ED patients than healthy controls? What about those with anxiety disorders? And if it is more prevalent among ED patients, why is that and what does it mean? How are they related? It will also be important to study whether misophonia is (or could be) involved in causing, maintaining, or exacerbating ED symptoms, and of course, how we can treat it, particularly in the context of eating disorders.
Finally, in Kluckow et al.’s study, only one out of the three patients reported misophonia symptoms to a therapist, which suggests that it might be wise for clinicians and therapists treating ED patients to screen for misophonia. Not only to further research on this topic but also to facilitate communication and enable patients to talk freely about their symptoms and how they may (or may not) affect their eating disorder.
References
Edelstein M, Brang D, Rouw R, & Ramachandran VS (2013). Misophonia: physiological investigations and case descriptions. Frontiers in Human Neuroscience, 7 PMID: 23805089
Kluckow H, Telfer J, & Abraham S (2014). Should we screen for misophonia in patients with eating disorders? A report of three cases. International Journal of Eating Disorders PMID: 24431300
Schröder A, Vulink N, & Denys D (2013). Misophonia: diagnostic criteria for a new psychiatric disorder. PloS one, 8 (1) PMID: 23372758
So interesting! I have had this problem since a young teenager, and the onset of my anorexia was after moving away from family to go to graduate school in a program that was not a good fit for me. I also have a history of anxiety. The severity has varied…I have had periods (perhaps during the worst of my ED?) where I would have to wear ear plugs during every meal and would cover my ears with my hair so my husband wouldn’t notice. Interestingly it also does vary by person…those closest to me seem to bother me the most? Currently I just sit through it and manage the anxiety with self-talk and wouldn’t call it a ‘trigger’, but rather something that is like nails on a chalkboard to me…
Interesting…
“Interestingly it also does vary by person…those closest to me seem to bother me the most?” That seems to be the trend in the studies I’ve quoted too. *Who* is making the noise seems to be important for many people in terms of *how* triggering/rage-inducing the sound is. (I wonder if it has to do with the fact that you expect the person to “know better”/be more considerate?). Do you find when you are the source of the sounds it is as bad as if its your husband who is making the sounds?
Thank you SO MUCH for writing about this! I have similar issues and feel like a complete lumatic that these noises aggravate me so much. I get triggered even by the sound of my own chewing bouncing around in my head. It make me incredibly anxious and throws me into fight or flight mode and I find it difficut to calm down. It’s one of my greatest challenges with eating. Anyway, thanks for addressing the issue. It’s helpful to know I’m not alone, even if there isn’t much research on it.
🙂
It is interesting you mention being triggered by the sound of your own chewing. Edelstein et al. found that something like 80+% of the participants in their study weren’t triggered when they themselves were making those noises. Is it just as bad if you are the one making the chewing noises as opposed to someone else? What do you usually try to do to calm down? What do you do in order to get through eating?
You are definitely not alone!
I also am disturbed by the sound of my own chewing, however, my reaction is different. Others chewing makes me fly into a rage, while hearing my own chewing makes me feel incredibly anxious/paranoid. What an interesting article! I have had this problem since I was a teenager and way before the onset of my ED. I always just thought I was crazy, and an asshole for my reactions to people eating/drinking and making other normal life noises.
It is very interesting to how many people can relate to misophonia! I never would’ve expected it. I wonder if your reaction to your own chewing (anxiety/paranoia) pre-dated the ED? And if so, whether it played into it? I can imagine that while misophonia and ED may be totally separate things, surely becoming anxious to the sound of your own chewing would probably have some effect on the ED.
The severity of my reactions vary from day to day and I haven’t been able to pinpoint exactly what makes them worse – but definitley days when there is more exernal stimuli in general around me are the worst. Oh smells are awful. If the food is very fragrant that make the noises completely torturous. My noises just make me anxious, where as the ones from others also make me feel panicky – like I’m being attacked and I do get more irritable – but I wouldn’t exactly call it rage. To try and calm down I’ve been trying to do more breathing exercises and meditation and keep up with a regular yoga practice which seem to help my overall level of anxiety. Food wise I try to stick woth softer foods and eat more of my food cold so it’s less fragrant and use minimal flavorings. I also eat by myself and make sure its as quiet as possible while I’m eating – like making sure I’m not doing laundry or anything that has other awful noises being produced at the same time. I also try to distract myself by looking at a magazine or surfing the net or doing something else that helps get my mind off the food. But obviously these are not strategies that one really wants to sustain long term… But so far it’s the best I got. I did just start taking dronabinol a few days ago which has really been helping to calm down the instant fight or fight responses i have and overall I feel less reactinve to noises and am not feeling as triggered by the smells either. So hopefully it will continue to help!
Thanks for your comment Sarah. It is all very interesting! And I hope some of those who read through these will feel less alone as a result.
I hope the dronabinol will continue to help as well! And yeah, like you said, strategies that work now don’t necessary need to be in place forever.
The sound of my own chewing is the worst for me – it’s the main reason I don’t eat. If other people are eating you can leave, but if I have to chew something and can’t drown it out with other loud noises, it’s like having to sit there with a spider on you.
It’s also generalized to onomatopoeias and food-related words. Has anyone else experienced that?
Weird thing I just realized, though, it doesn’t so much bother me when cats are eating. Maybe it’s because they’re small? I’ve often wondered if the underlying cause of this is some ancestral memory of hearing dangerous animals eating your comrades in the woods.
Wow, this is interesting.
I had my ED for several years around twenty years ago. I don’t recall experiencing irritation and rage around noise then. But I certainly suffer from it greatly now.
What bugs me …
–any repetitive noise such as a ticking clock (even if faint).
–people slurping drinks.
–someone eating while they are on the phone to me (chewing in my ear).
–throat clearing.
–my housemate talking on the phone.
–my housemate’s radio or TV.
–other people’s music.
I often wear earplugs or listen to music through earphones to block other people out.
I also have a big problem with repetitive visuals such as flashing lights on gadgets (I have black tape over LEDs on my laptop and in my car), and animations on web pages.
I suspect in my case that the noises and visuals are connected. They absorb almost all my concentration and I can’t relax until they stop.
Hmm, interesting. So the onset of these symptoms came after you had already recovered from your ED? Do these things just ‘bug’ you (I mean most people would be annoyed at what you describe) or do they make you rage? I find all of those noises distracting (I used to wear earplugs in the house even when I was alone!), but not rage-inducing. The potential link between the visuals and the noises is also interesting. In the Edelstein et al study it seems the misophonia participants didn’t find visuals triggering, so I wonder, if there is a connection, where exactly it may be. Ah, we know so little about this subject that it is all mostly just speculation at this point. It will be very interesting to see the research that comes out on this topic in the next few years.
If I believe there is an element of disrespect involved, I feel rage. If I suspect someone is thinking ‘F*ck you, I’ll do what I want,’ then yes, rage. If I ask someone to stop and they don’t, rage. Otherwise, as in the case of, say, a ticking clock, then the experience is that I can’t concentrate on what I’m doing because I am SO aware of the disturbance. No rage.
The visuals, such as a cursor on a screen flashing on and off, are like the ticking clock. I take the batteries out of other people’s clocks. And I select words to stop the cursor flashing. No rage.
I am a perfectionist (very ED, I think?), and just want everything to be peaceful and in order. I think that might be the connection between the noise and the visuals?
“I am a perfectionist (very ED, I think?), and just want everything to be peaceful and in order. I think that might be the connection between the noise and the visuals?” That’s an interesting thought! Perhaps it could be, I really don’t know.
The point about suspecting disrespect seems to be something that’s echoed by others in the papers as well.
Wow, I had never heard of misophonia, but after reading the associated article mentioned it was like reading about myself! So interesting to see that this is an actual condition. Especially as it runs in the family along with all the OCD stuff.
Indeed, it is interesting! I’m not sure to what extent it runs in families though; it is hard to say given that there’s so little research. It *seems* that it may run in families but we’d need more research to really confirm that.
Thanks so much for posting this! I learned about misophonia while working in a doctor’s office during the first year of my recovery. It rang so true for me, but I never realized there had been any study of the link between misophonia with EDs. This sheds a lot of light on what I experienced during my ED and while first recovering.
I was very sensitive to sounds like vacuuming and dishes being clanked (especially when the dishwasher was being loaded or unloaded), so much so that I usually had to leave the room if someone was doing either. I was a grad student living at home during the time, and since my family doesn’t eat together very often I would eat most of my meals by myself. For some reason, my mom had the habit of deciding to do kitchen chores whenever I happened to be eating lunch or dinner. The house would be quiet for hours, but when I would finally creep into the kitchen to make myself a meal, she would seemingly instantly decide that that was the time to come out of her room to completely clean out the refrigerator, empty a sink full of dirty dishes, stack dishes, vacuum the kitchen floor, etc. Now I realize she probably wasn’t doing this to purposefully be annoying (maybe the sounds of food prep in the kitchen cued her to remember the chores), but at the time I perceived it as beyond rude; extremely frustrating and excruciating.
I was already struggling to eat, and trying to do so with loud noises in the background made me extremely anxious, to the point where I had to eat my meals in my bedroom or even leave the house to eat outside if I could. I tried to explain it to her but since she didn’t know about the ED, there was only so much I could share. Now that I have another year of recovery behind me, I’ve noticed the misophonia is so much better. Those sounds still annoy me and are not my first choice for a dining soundtrack, however they bother me much less now that I’m generally way less anxious around food. I’m also weight restored/stable and cognitively speaking, ED-thought-free about 90% of the time on the average day, so I wonder if those factors may be related to the increased ability to tolerate unpredictable sensory stimuli.
Thanks again for the great article! I don’t feel so weird anymore 🙂
Thank you for your very interesting article! I was pleased to see a name for this affliction, as well as a rise in interest in it. My sister and I both have difficulty with many noises, most of them commonly associated with eating. My sister however, suffers more than me. Are there any studies active in the toronto area? We would love to be a part of something to help gather more information. Neither my sister nor I have suffered from an ED or any anxiety disorders.
Ive just stumbled accidentally onto this and am pretty sure that I have in some way shape or form an ED and misophonia. For years (since I was very young maybe about 6 or7) I have suffered with noise rage as I called it, I always put it down to my anxieties and as i grew older it became harder to control and the list of noises and actions grew longer.
I have to sit facing a window in a restaurant so i cant see others eat…I have quite often had to leave the area and have even been known to burst into tears. The effect over the years I feel has had an adverse one on both my eating habits and my family.
I tend to binge eat when people aren’t around to HEAR me..I can eat when around other people but i am super sensitive to my own eating noises too.
i have a list of noises from snoring and spitting to heavy breathing, whistling, chewing (especially with the mouth open) and dont get me started on people with poor table manners..infact my anxiety level rises as I am writing this. A metalic taste in my mouth and …… Im back (needed a break). hopefully a bit more research and the feeling of wanting to punch somebody really hard or scream at them for their noises, will help me cope better than I have been.
I have an ED and my boyfriend has misophonia. He complains about me eating and drinking too loudly and it makes me very self conscious to eat in front or around him and now I hear every bite I take. Whenever he snaps at me for making too much noise I find it very triggering for my ED.