Eating disorders are rarely static. Symptoms fluctuate, waxing and waning as circumstances change. Often, these fluctuations lead to diagnostic crossover–between subtypes of one disorder or to a different eating disorder altogether. The heterogeneity of symptom severity and frequency led to the establishment of the “eating disorder not otherwise specified” diagnosis in the Diagnostic and Statistical Manual. Essentially, it is everything that doesn’t quite fit into the “anorexia nervosa” or “bulimia nervosa” categories. (For example, I would guess that it is a common diagnosis for patients who fail to meet the “amenorrhea” criterion for the AN diagnosis.)
ED-NOS is a category for everything that doesn’t conform to some rather arbitrary criteria required for bulimia nervosa and anorexia nervosa, meaning: it is the diagnosis for a lot of people. Okay, that’s not very scientific, I know, but I wouldn’t trust these numbers anyway–usually people who fall into this category don’t feel “sick enough” to seek treatment, in the USA they have difficulty getting treatment coverage, and many just don’t think they have a problem (and nor do those around them). I know a fair number of people who fall into this category.
Maybe they haven’t lost quite enough weight, or they don’t binge and purge 2 times/week–maybe it is just once a week but the rest of the week they fast. Maybe they are eating a normal amount of calories but it is limited to a handful of foods that are “permissible” in that person’s mind. What if their body, their weight, the calories they consume rule their life–in the sense that it determines how they feel, what they do, who they interact with and how often, and so on. How about if they don’t binge but purge every normal meal they eat and yet maintain a weight above what is required for the AN diagnosis?
I think most clinicians (certainly most women and men with EDs) wouldn’t hesitate to say that individuals who fall into those categories have an eating disorder. They could be on their way to fulfilling the full diagnostic criteria of BN or AN, or they could be transitioning from one disorder to another, or this is just how their eating disorder manifests.
Right now, these hypothetical individuals would be lumped into the ED-NOS category. But there are several problems with the ED-NOS diagnosis , several of which are outlined in the box below.
- It is clearly not a useful diagnosis: diagnoses are meant to provide a meaningful description of the condition, ED-NOS doesn’t.
- Individuals with ED-NOS often feel like their disorder isn’t “real”, “severe enough”, or warrants professional help. (Nothing could be further from the truth.)
- Insurance companies often don’t cover it (perhaps because it is perceived as less severe?)
- DSM guides research (an AN group is selected based on fitting the DSM criteria, for example). But how useful or representative are these findings if most people don’t fit neatly into these groups?
- More importantly, how useful are they if they might fit into it at the time of the study’s recruitment but not 3 weeks later?
Given that the new edition of the Diagnostic and Statistical Manual is due to come out in 2013, it is necessary to evaluate the validity and utility of the current classification categories, and change accordingly.
This is precisely what Eddy et al. sought to do in their 2008 paper titled “Diagnostic Crossover n Anorexia Nervosa and Bulimia Nervosa: Implications for DSM-V”.
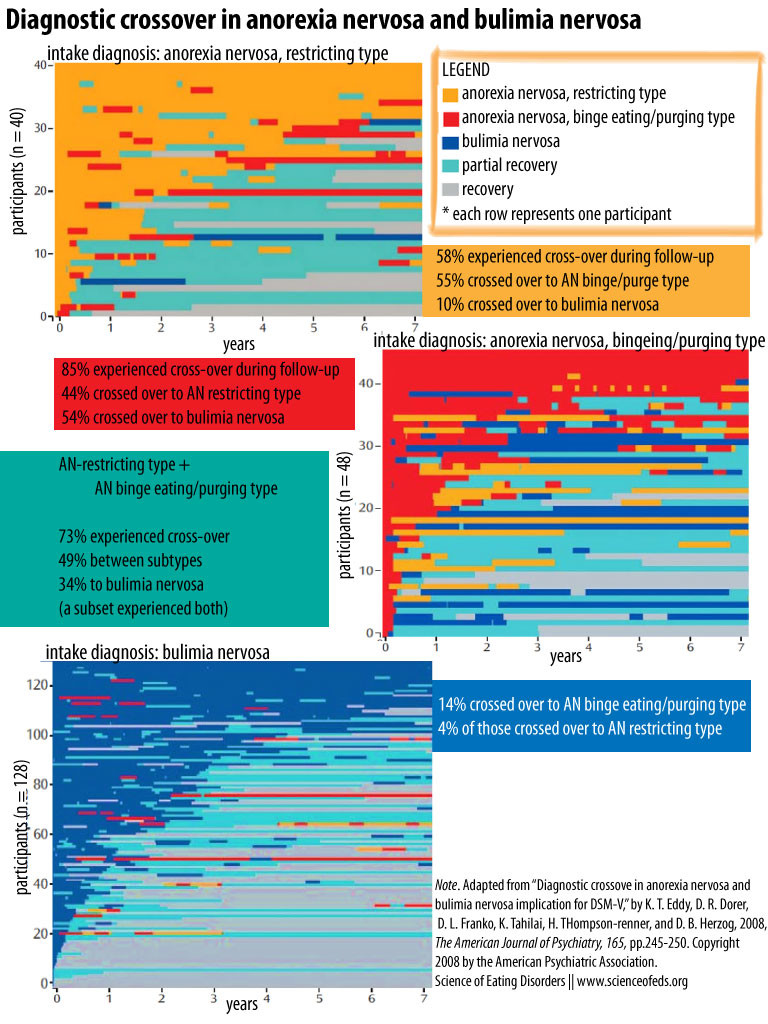
Individuals were grouped based on their initial diagnosis (AN-restricting type, AN-binge eating/purging type and BN) and followed weekly for the next seven years. Here is summary of what they found (click to enlarge):
The results are not surprising to me, but it is nice to see them in print.
There are some things that you might be wondering about: partial recovery and full recovery rates seem pretty high, what gives? Well the mean sample age was almost 25 years old (the AN patients were slightly younger than the BN patients, interesting to note, given that AN to BN transition was more common (this relates to my issue with the author’s conclusion). But most importantly: the mean duration of the illness at intake was 6 years for AN and 6.7 for BN. That’s a considerable amount of time, which may explain the relatively high partial and full recovery rates–and yet at the same time, highlights just for how many people an eating disorder is a lifelong battle (not necessarily in symptoms but mentally). This is especially true when you consider that all of the participants were seeking treatment.
My own experience falls very much in-line with this study’s findings: diagnosed with AN-R, following partial recovery, back to AN-R, partial recovery, AN-BP, AN-R, AN-BP, BN, partial recovery (a.k.a., beginning of restriction and weight loss), AN-R, AN-BP, AN-R, AN-BP, BN, partial recovery/symptom remission. Okay, that’s not exact, but pretty damn close.
I think this study brings to light the difficulty of studying eating disorders. But at the same time may explain why the field has been relatively unsuccessful in finding genes that are highly correlative to a particular disorder. That’s not something I’d expect to find give that eating disorder symptoms (and diagnoses) fluctuate over the duration of the disorder. And how useful are the studies that focus on that minority population that do not experience diagnosis crossover?
With regard to the first question, I think you are more likely to find correlations between specific personality traits than particular symptoms. That’s just my hunch. With regard to the second question, I think this is the best we can do at the moment but presumably, if we study the minority non-diagnostic crossover groups, we will be able to extrapolate into that more diagnostically heterogeneous majority.
One main shortcoming of this study: only women diagnosed with AN or BN at intake are included because the ED-NOS category was not established when the study began. The authors also note the need to differentiate between ED-NOS and partial recovery (I fully agree!).
I have one issue with the conclusion that Eddy et al. (and others) come to:
These findings support the longitudinal distinction of anorexia nervosa and bulimia nervosa but do not support the anorexia nervosa subtyping schema.
I’m not so sure: the average duration of the illness prior to the commencement of the study was 6-7 years. Certainly it is conceivable (and I would argue the findings would support this) that many of the women that at the beginning of this study were diagnosed as BN, or even AN-BP, initially struggled with AN-R (perhaps even for years).
I’m quite interested in this topic and there are several good articles on how the DSM-V diagnostic criteria should change and the implications of particular changes. This group has some more recent articles published, following up on this, and I hope to cover them in future posts.
References
Eddy, K.T., Dorer, D.J., Franko, D.L., Tahilani, K., Thompson-Brenner, H., & Herzog, DB,. (2008). Diagnostic crossover in anorexia nervosa and bulimia nervosa: implications for DSM-V. American Journal of Psychiatry, 165 (2), 245-250 PMID: 18198267
I don’t find these results surprising, based on my and others’ personal experiences. But it’s nice to see them actually published in a paper! The media and the scientific community like to make you think that diagnoses are usually static.
I wonder what these findings will have on research previously done on EDs, particularly those on personality traits that will predispose you to certain EDs. Personality tends to be pretty stable over time, but ED symptoms aren’t. Yet the research on personality show anorexia and bulimia having many traits that are the complete opposite. How valid are those results if it’s common for people to switch between disorders in as short of a time as just a few months?
Weight is also a big determinant in what diagnosis you get. What if two people go through the exact behaviors, and one becomes underweight and the other one remains overweight due to a metabolic disorder. Why would research suggest they are likely to have a different set of personality traits when it’s possible that both people could have had the same diagnosis if the physical disorder wasn’t present in one of them?
Really good questions! I’m working on a post on the continuum model of EDs that may address some of the points you raise, in part – rather than positing diagnoses as discrete disorders or binary opposites, it could be possible for individuals to shift along the continuum over lifetime – but that doesn’t necessarily answer those questions satisfactorily. Hmm.
I’m not sure how stable personality actually is. Is it as stable as we think, or is it just our prefrontal cortex piecing it together, making a story and post hoc rationalizations for why we did the things we did and why we do the things we do?
With regard to your second paragraph, I find that my personality traits and behaviours change markedly with symptom fluctuations. So, I don’t think these things are stable. I think there’s what we tend to do when we are not under any kind of stress and what we do in stress/high anxiety situations (different stressors can lead to different symptoms), and then there’s EVERYTHING in middle of those two extremes. I think every person probably has some stable middle, a mean, in terms of personality traits – you know when you feel you are “you”? On a spectrum of personality traits, or on a Cartesian plane, whatever, everyone probably has some area in which they oscillate under normal conditions, a mean with their own standard deviation. But the mean, and the standard deviation changes under stress, probably in a predictable way, depending on normal conditions. It is hard for me to put on paper in a clear way, but hopefully you know what I mean.
I think the problem comes with assessing people at one time-point. BN individuals are like this, AN individuals are like this. But really, it should be, when you are bulimic, you are more likely to exhibit these types of personality traits, and so on.
I’ve had an eating disorder since I was 15 1/2 years old I am now going to br turning 30 in may2013! It started full blown AN, after having AN for 6 months I was hospitalized for only about 2 weeks. I was nowhere near “ok” & my parents had NO idea what an eating disorder was! I had no idea either but ended up changing into ANBP:-(! I have now lost 6 teeth and counting from this relentless disease, just one of the many side affects! I didn’t realize I still had ANBP I just thought I had been doing ok which was better than I was when the AN first started boy was I wrong! It comes and goes sometimes the AN (which id much rather have) is stronger and sometimes it’s ANBP which I dread! I have tried to find help since turning 29 years old! I have a daughter now and I’m really scared I’m not going to be around much longer! I’ve tried to get into a therapy group, the only one is 2 hours away! If anyone knows of any free help, as I have no money to pay for treatment unless someone knows a place that takes “County Medical” I live in Oakley,Ca,, I would be more than grateful for any help! Thank you!
P.S.-If there are any study’s that need patients I’d be more than willing to help out, I would do anything for someone to find out anyway for another human to NOT have to go through what I’m living with!
Hi Courtney,
Thank you for your comment. I’m really sorry to hear about everything that you’ve had to go through with you eating disorder.
It is also terrible that access to treatment is so poor where you live 🙁
Getting involved in research is one way to get treatment without having to pay for it (and often/usually get compensation, actually, depending.) I would suggest maybe looking at Universities that are a reasonable distance from where you live? Then you may be able to get both some treatment and help researchers out as well.
I’m not from California, so I don’t know what’s around you unfortunately. Maybe San Fran?
Tetyana