Nurses can play an important role in facilitating recovery from anorexia nervosa, particularly in an inpatient or residential treatment setting. But what makes a good nurse from the patient’s perspective? More specifically, what qualities do adolescents with anorexia nervosa consider important and helpful during recovery?
The answer may seem obvious: understanding, empathetic, supportive, non-judgemental, and the like. But those are sort of general characteristics that apply to good friends, family members, partners, doctors, other healthcare professionals, and even teachers.
Joyce von Ommen and colleagues wanted to dig a little deeper than that. They wanted to find out what components of nursing care helped patients restore normal eating and exercise patterns.
In order to find out, they collected interviews from 12 female adolescent patients (mean age of 15, range from 13-17), who were discharged from a specialized eating disorder treatment centre within three months of the interview. The patients were diagnosed with anorexia nervosa and were in the hospital for an average of almost 19 weeks (range: 9.5 – 35.5). Using semi-structured interviews, they began by asking participants what helped and hindered their weight recovery and then moved on to discuss other aspects of nursing care.
My first problem with this paper is in the methods section: there is no mention of who did the interviews. Why is this important? It is important because because all of the co-authors of this paper, with the exception of Annemarie van Elburg, are registered nurses. If this information is known to the interviewees’ I think there’s a much higher chance of biased answers.
A biased answer is an untrue or partially true statement. Bias influences and skews answers, masking truth. An untrue statement can be intentional or unintentional. It doesn’t matter; it is bias. And it happens for various reasons. (source)
Here are a couple of biases that might arise if the interviewees’ are being asked about what makes a good nurse by nurses.
Moderator Acceptance Bias: Some respondents provide answers to please the moderator. Respondents interpret what they believe the moderator wants to hear and their answers may be false. If answers don’t ring true, challenge them in a friendly way. Don’t reveal too much about yourself.
and to a lesser extent
Social Acceptance (Desirability) Bias: Respondents provide socially acceptable answers that may be false. People say what is socially acceptable, even though they may feel or think something else. They may twist the truth, or offer half-truths. (source, same as above)
Think about it, if you were being asked what makes a good nurse by your friend, chances are, your answers would be different than if you were to talk to a nurse. Of course, that’s not always true and it may not be true for everyone, but we are talking about biases that might affect the data as a whole, because we are talking about a group sample.
Anyway, I find this problematic. It would be helpful to know who did the interviews, particularly because the responses seemed very positive.
So, what where the responses?
Well, first, the authors divided the period that the patients were inpatient into three phases and asked the participants to detail how the nurses helped the patients achieve the goals in each of the phases.
The initial phase was immediately after admission, where patients have to get used to the treatment rules and structure. The second phase characterized by trying to integrate a bit of decision-making on the part of the patient and normalcy (ie, going back to school, doing recreational activities). In the final phase, patients were being prepared to integrate back into normal life and regain even more responsibility over eating and exercise regimes.
PHASE I
In phase I, participants reporting feeling a mixture of anxiety about eating and weight gain, but also relief that they no loner had to make decisions about eating and exercise: it was up to someone else. According to van Ommen, the patients felt that the nurses presence at all times, as well as the complete removal of all decision-making responsibilities was crucial, and indeed necessary to break the eating disorder habits.
In retrospect, the patients regarded the directional actions of the nursing staff as very helpful. They told the interviewers that they had lost all sense of how to eat properly and that they had needed the structure-based interventions to be able to resume their normal eating pattern. They had to relearn how to eat…
It was a good thing that someone took over so that I did not have to think for myself. Just so that I did not have to make any decision at all. (patient 5, age 15)
Interestingly, van Ommen and colleagues write that participants reported the importance of finding out about the negative consequences of restriction, starvation and anorexia nervosa in general from the nurses. I’m surprised by this, as it is kind of (though not completely) contradicting (or at least, not aligning) with the findings I reported in my previous post (see Table III). This is just one of the many instances which makes me question whether the participants were responding truthfully or just responding the way they thought they ought to respond.
Finally, participants also said that being in a group setting among others with anorexia nervosa was a positive factor in re-learning how to eat, particularly by observing how others were eating and not experiencing anxiety, so perhaps they shouldn’t either. In these scenarios, nurses were seen as crucial in facilitating interactions between patients, particularly between those in more advanced stages with recovery with those in the earlier stages. (By the way, I’ve blogged before about how group settings can actually be more harmful then helpful, here.)
PHASE II
In phase II, nurses were seen as role models in helping patients gain a better understanding of normal eating and exercise habits. Particularly, nurses were there to support patients when patients began to have more autonomy over their food choices, by guiding and discussing the food choices with them. According to the patients, the nurses were seen as key figures in guiding and encouraging them to begin to take responsibility for their meal plans (but yet they were there when the patients felt lost and needed guidance.)
[Patients] wished to return to a normal life, but still felt deeply anxious about consuming food and gaining weight. To reduce that anxiety, patients indicated how important it was for them to still receive in-depth information about eating disorders. Modelling also proved to be very important in this phase. The nurses acted as role models by joining the meals and showing a normal eating behaviour, but also by participating in recreational activities. For instance, they showed patients what was considered a normal pace of cycling and that it was perfectly normal to stop cycling to take shelter from the rain.
I am probably really wrong here, but I find the tone of this paper very, almost dismissive, of the gravity of the eating disorder. While losing the sense of “normalcy” with regard to eating and exercise is certainly common, and definitely something I’ve experienced, I feel like framing it as solely a problem of “not knowing what normal is” to be rather, dismissive? Just knowing what “normal” is doesn’t mean that suddenly the patients stop feeling anxious about not going above and beyond normal. Knowing what “normal” is doesn’t suddenly negate the drive to exercise, to under eat, and so on..
PHASE III
In the final phase, patients relied on the nurses for continual support and counselling to help them prepare to settle back into the “real world.” In this stage, the nurses also helped patients “put things in perspective,” particularly with regard to eating, body image, and exercise issues.
The structure and decision-making that the nurses were wholly responsible for in the initial phase were reduced, and the nurses instead allowed the patients to make their own decisions and “find their own solutions to problems they encountered.” However, the nurses were still there, and still focused on the patients, which helped the patients practice their newly learned skills without the fear of adverse outcomes.
The respondents highlighted the importance of being trusted by the nurses, since that made them aware of their own potential and increased their self-esteem.
Finally, the nurses were seen as an integral part to helping the patients develop and discover “the person behind the eating disorder.”
They felt especially supported by an attitude of respect and equality by the nurses. The patients noticed that their eating disorder was no longer the only topic of conversation and that they were preoccupied with other things, such as being in love, using makeup and having fun.
The participants felt that the nurses actively contributed to the development of the patient outside of the eating disorder by stimulating the patients with new challenges and “humour.” (Yes, it says “humour”.)
On a more positive note, von Ommen and colleagues conclude that it is clear from this paper that nursing eating disorder patients is “specialist work” and that it is “essential” that nurses receive advanced training to be able work with this population. This is particularly so because working with eating disorder patients, beyond all the other challenges, also requires constantly reassessing the patient’s strengths, weaknesses, place in recovery, and emotional/psychological status, perhaps more so than in many other disorders.
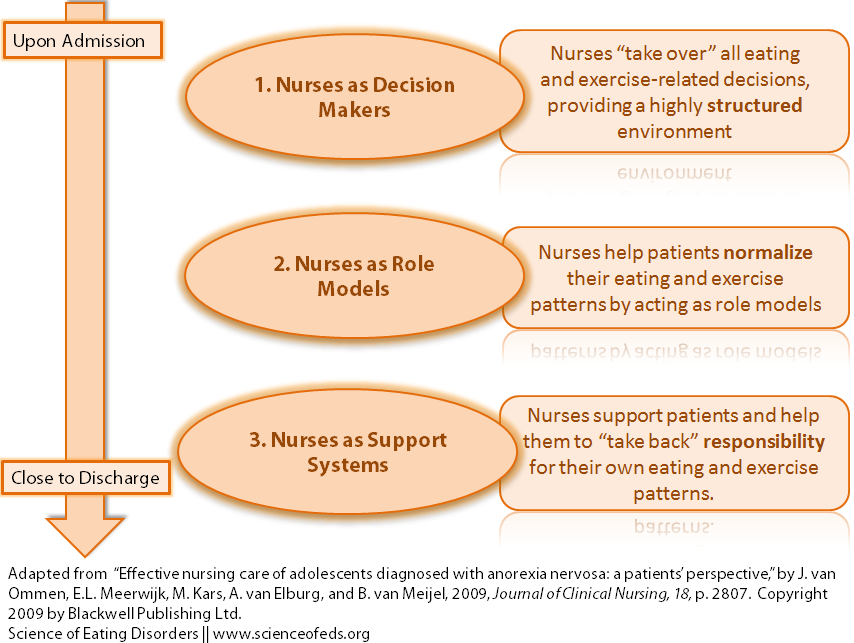
In the figure below, I summarized and adapted figure 1 from the paper, which essentially details the “central aspects” of nursing care that adolescents with anorexia nervosa identified in this study.
All in all, I am honestly not really sure what to think of this paper. It seems eerily too positive and discordant with all the personal anecdotes that I’ve read in all the years I’ve spent browsing and being part of online eating disorder communities. Really, everyone thought the patients were awesome? Undoubtedly for some, the nurses were overwhelmingly a positive influence (which is great!) but I wonder if the positive responses were exaggerated due to some of the biases I mentioned above, or perhaps due to retrospective bias (like, remembering the good parts, forgetting/minimizing the bad?). Perhaps this is because only twelve adolescents were interviewed in this study? Or perhaps the treatment centre is just amazing. I don’t know.
I don’t want to be too critical, too sceptical of the findings, but a part of me definitely feels like the authors either didn’t try, or tried and failed, to find dis-confirming evidence (that is, examples that contradict their model.)
Readers, what do you think?
Are you convinced or somewhat sceptical?
Do you agree with the participants in this study? What have your experiences with nurses in eating disorder treatment centres/inpatient units been like? What were some helpful things they’ve done, harmful? I’ve love to hear your feedback!
References
van Ommen, J., Meerwijk, E.L., Kars, M., van Elburg, A., & van Meijel, B. (2009). Effective nursing care of adolescents diagnosed with anorexia nervosa: the patients’ perspective. Journal of Clinical Nursing, 18 (20), 2801-8 PMID: 19538553