The first published case of a late-onset eating disorder (at the age of 40) was in 1930 by John M. Berkman. In 1936, John A. Ryle published a case study of an eating disorder in a 59-year-old woman. Just how common are eating disorders in late middle-age or elderly individuals?
One study of 475 community dwelling elderly women aged 60–70 years found that 3.8% met diagnostic criteria for eating disorders. A study of elderly Canadian women reported that symptoms of disordered eating were present in 2.6% of women aged 50–64 years, and in 1.8% of women aged 65 years or older (Gadalla, 2008). In an investigation of eating disorders in elderly outpatient males, a minority (11–19%) who were undernourished were found to have abnormal eating attitudes and body image, including inappropriate self-control around food (60%), unsuitable eating attitudes (26%), and distorted body image (3–52%) (Miller et al., 1991).
There aren’t a lot of studies on this topic, but the the above figures illustrate that there’s a significant minority of elderly individuals who struggle with eating disorders or disordered eating.
What causes or precipitates eating disorders in late adulthood? Well first, it is important to keep in mind that a proportion of eating disorders in late-life occur in women who either never recovered from their early onset eating disorder or in those who had a remitting/relapsing ED pattern throughout life. But many do develop eating disorders for the first time in their 50’s, 60’s, and 70’s.
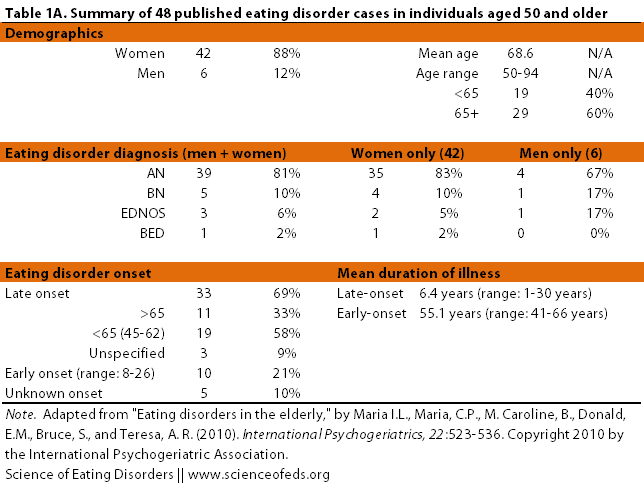
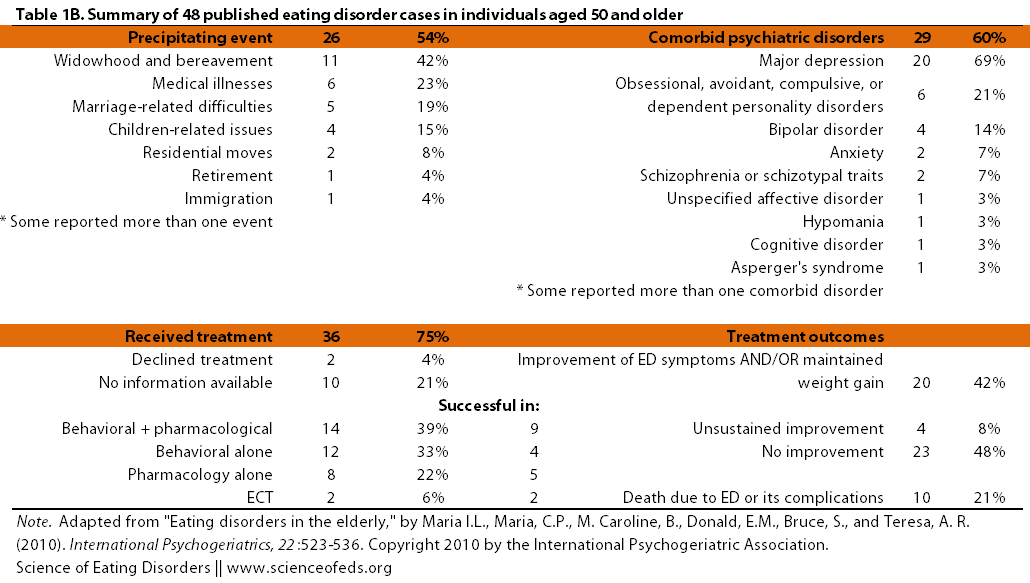
In 2010, Maria Lapid and colleagues published a review paper of all the published case studies of eating disorders in individuals over the age of 50. They found 48 studies. I’ve summarized the findings in the tables below:
(Click to enlarge.)
Thirty-three out of the 48 individuals had late-onset eating disorders, with 11 having an age of onset above 65. Precipitating stressful events were only noted in 54% of the cases, and even then, we can never be precisely sure of the role those events had in the eating disorder. It is interesting to ponder about what could cause (or predispose) someone to engage in restrictive eating or bingeing and purging in late age.
Though, to be honest, I think the topic is more interesting if you think EDs are almost exclusively for vain teenage girls. Once you let go of that idea and realize that restricting and/or bingeing/purging are powerful methods of regulating mood and emotion, it is really not that surprising that individuals of all ages develop EDs.
An aging physical appearance, with age-related body changes, and changes in familial relationships are associated with the development of eating disorders in the elderly (Gupta, 1990). In a study that examined the relationship between apprehension about aging and a drive for thinness in men and women, a direct correlation was found between concerns with the effect of aging on appearance and the level of preoccupation with weight, dieting and exercise (Gupta, 1995).
Other proposed causes of eating disorders in the elderly include the need for control and a plea for attention. Older adults with eating disorders may use eating as a control mechanism to regain power in their lives, a consequence of the loss of control that accompanies aging (Harris and Cumella, 2006). For some, eating disorders are a method of gaining control over loved ones through protest and by drawing attention to the discontent they feel for their current circumstances (Harris and Cumella, 2006).
[…] Precipitating events such as personal losses and life changes magnify the sense of loss of control in the life of an older adult, and eating disorders may be a method of coping with these stressful events (Cosford and Arnold, 1992).
I do wonder, if we sometimes assign more meaning to behaviours than is really necessary or justified. Maybe for some individuals, it is just about reducing anxiety or feeling a little numb? Maybe for many, eating disorders began after loss of appetite due to other medical problems or medications? As a side note, while I think it is important to be aware of possible causes and risk factors, I think it is more important to focus on treatment than to mine for the ultimate causes of restriction and/or bingeing and purging.
But moving on. The fact that most of the case reports presented in this paper were of individuals diagnosed with anorexia nervosa isn’t surprising. The cases date back to 1936 and bulimia nervosa really came into the diagnostic nomenclature in the 1980s. Moreover, AN is easier to spot and harder to hide.
What is depressing, but again, not surprising, is that improvement in ED symptoms and/or weight was observed in only 20 cases (42%), whereas death due to the ED or its complications occurred in 10 cases (21%). Unsurprisingly, a combination of behavioural and pharmacological therapy seemed to be the most successful.
It is really important to remember that this review is a summary of published case studies. It is not necessarily representative of eating disorders in the elderly. In fact, it almost certainly isn’t representative. This is because many patients whose EDs might not be severe enough to catch the attention of a medical doctor can easily go unnoticed. Most of the cases reported here were recognized during hospitalizations, and so it is reasonable to assume that many patients who are not quite sick enough to be in need of hospitalization go unnoticed.
RECOGNIZING EATING DISORDERS IN THE ELDERLY
Recognizing eating disorders in elderly patients can be challenging. For one, weight loss can be a symptom of many different medical illnesses or it may be the result of medications. It becomes imperative to take a really careful patient-history and to consult with family members to get a complete picture of the patient.
One really concise screening questionnaire is called SCOFF. It is (apparently) 100% sensitive if the answer to two or more questions is “yes”:
When it comes to treatment, a combination of behavioural and pharmacological therapy seems to work best. However, treatment has to be tailored to the individual. Moreover, close follow-up is crucial to ensure compliance and continued remission. Whenever possible, family members should be involved and encouraged to take a role in the recovery (supporting the patient through meals, etc.)
Eating disorders in the elderly present in many of the same ways they do in adolescents and young adults. And treatment often looks very similar, too. However, there are potential issues that are unique to this population:
- Family, most often, means spouse or children, as opposed to parents (which may or may not be a good thing)
- Comorbid medical illnesses might complicate ED diagnosis and treatment (for example, when weight loss is caused partly by a medical condition and in part by an ED)
- Elderly individuals are often on many different medications, which must be taken into account when prescribing other medications to avoid adverse effects/drug interactions
- Medications that reduce appetite should be noted (and changed, if at all possible)
- Cognitive impairment may limit the utility of many behavioural therapies (such as Cognitive Behavioural Therapy)
- Hearing or vision loss, which is common in old age, might pose problems in treatment as well, such as group therapy, and should be taken into account
In the future, I’d love to see more controlled studies that examine the prevalence of eating disorders and disordered eating in the elderly population and examine the efficacy of different treatments. In the meantime, I think family members will continue to play a crucial role in bringing up eating disorders as a potential differential diagnosis to the healthcare providers, who, for the most part, are probably unaware that eating disorders can occur at any age.
PS. I will probably be posting less in the next week to week and a half as I have to prepare for my defence.
References
Lapid, M., Prom, M., Burton, M., McAlpine, D., Sutor, B., & Rummans, T. (2010). Eating disorders in the elderly International Psychogeriatrics, 22 (04), 523-536 DOI: 10.1017/S1041610210000104

At my first time in outpatient (age 14), i remember being placed in group therapy with a man in his 60s and finding it very odd that there was no differentiation in treatment. It must have been really difficult for him to deal with both the age and gender stigma while being put into group talk therapy with predominantly 13-16 year old girls. A few of the girls were as young as 7-11 years old. How effective can that treatment really be for him?
In all forums discussions and studies are made about poor intake of food by elderly. I have a different case. My mother who is 88years demands food every two to three hours be it day or night. She talks properly, walks around and has no health issues or illness. No proper sleep during night so eats two three times after 9 pm. if we refuse to give she behaves like fainting and shows breathing difficulty and fatigue. Once she gets food she becomes normal. during all meals portion size is normal.She doesn’t have diabatics,BP etc. what could be the reason. discussed this with our doctors and they don’t have an answer. She also has health drinks like Ensure and protinex every day. Hope there is a solution to this issue