The challenges of treating anorexia nervosa are plenty; some of these challenges — like low prevalence rate and high treatment dropout rate — make conducting randomised controlled trials aimed at identifying effective treatment methods really hard as well.
So I was pretty excited about the recently published randomised controlled trial comparing focal psychodynamic therapy (FPT), cognitive behaviour therapy (CBT), and optimised treatment as usual in adult (a harder to treat demographic than adolescents) anorexia nervosa patients.
Reading the paper, I was pretty impressed with how good the study design was; I’m not going to go into all the nitty-gritty details, but if you have access to and the chance to read the paper, do it. You’ll appreciate, I think, the amount of effort that went into this.
THE STUDY
Patients were recruited from ten universities across Germany. They had to be adult females with a BMI between 15-18 and with no current substance use, psychotic or bipolar disorders. In total, 242 individuals started the study (80 in the FPT and CBT groups, and 82 in the treatment as usual group). I’ve summarized what the treatments entailed below.
SUMMARY OF TREATMENTS PROVIDED
All treatment was provided by physicians and psychologists who specialize in treatment anorexia nervosa and the treatment method provided. The treatment duration was 10 months (an average of 40-45 sessions).
Focal dynamic psychotherapy
- Identified psychodynamic foci; treatment can be roughly divided into 3 phases:
- Phase I: Development of therapeutic alliance, focus on pro-anorexic and ego-syntonic beliefs, self-esteem
- Phase II: Main focus on relevant interpersonal relationships and association with eating disorder behaviours
- Phase III: Transfer/apply concepts to everyday life, anticipation of treatment termination, and parting
Enhanced cognitive behaviour therapy
- Treatment consists of modules and includes homework assignments
- Overarching theme is a focus on improving self-efficacy and self-monitoring
- Main modules focus on motivation, nutrition, and relapse prevention
- Other modules focus on cognitive restructuring, regulating mood, self-esteem, and improving social skills
- Includes educating patient on dangers of being underweight, and helps patients initiate and maintain healthy eating
Optimised treatment as usual
- Patients received support in accessing established psychotherapists who had experience working with eating disorder patients
- Family doctors took weight measurements and blood work and were asked to admit patients to hospital if their BMI fell too low.
- The type of therapy and amount of therapy was not regulated in this group
PATIENT DEMOGRAPHICS AND CLINICAL CHARACTERISTICS
The average age of the participants was 28, the average BMI ~16.5 (~70% were <17.5, and 30% were between 17.5-18.5), and about 60% had been struggling with their eating disorder for 6 years or less. With regard to anorexia nervosa subtypes, there was almost a 50/50 split, with slightly more patients with the restrictive-type.
Dropout rate was 30% by the 12-months follow-up (as Dr. Cynthia Bulik stated in her commentary on this article, “compared with other anorexia trials, this dropout rate is quite good”).
SUMMARY OF MAIN FINDINGS
There were no differences between treatment groups in weight gained by the end of treatment and after the 12 months follow-up.
The average increases in BMI were 1.6, 1.4, and 1.2 in the FPT, CBT, and treatment as usual group, respectively. There were no differences between groups in eating disorder psychopathology at the 12-month follow-up, and the researchers did not find any differences in treatment response between restrictive and binge-purge type AN patients.
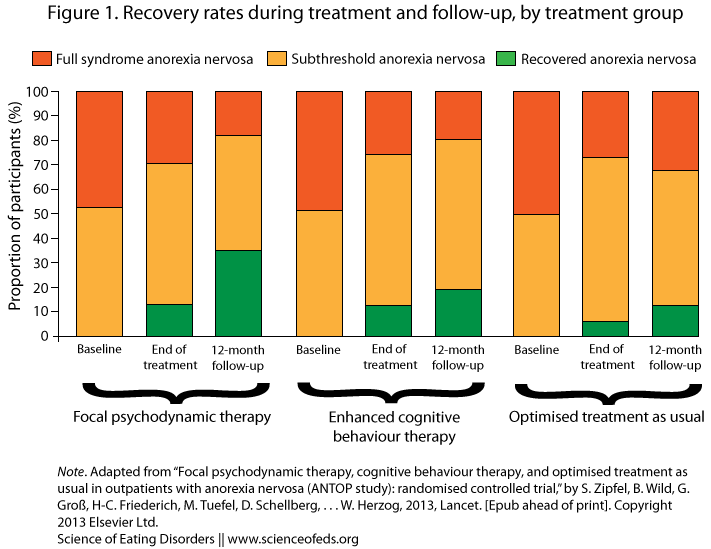
The figure below shows the proportion of individuals in each group that had full syndrome, partial syndrome (subthreshold) and those who had achieved recovery at the end of treatment and 12 months after treatment ended.
Recovery was defined as a BMI greater than 18.5 and a score of 1 or 2 on the psychiatric status rating scale, based on the patient’s score on the ‘Structured Inventory for Anorexic and Bulimic Syndromes’.
There were some differences. Patients who had a starting BMI of <17.5 had gained more weight by the end of treatment in the CBT versus FPT group (17.5 versus 16.9). And, importantly, at 12-month follow-up, 35% of the patients in the FPT group, versus 13% in the treatment as usual group, had achieved recovery.
During the duration of the study, 23%, 34%, and 41% of patients in the FPT, CBT, and treatment as usual groups, respectively, received inpatient care. That said, no serious adverse events occurred during the trial period as a result of weight loss.
At the 12-month follow-up, 21%, 22% and 28% of patients in the FPT, CBT, and treatment as usual groups, respectively, still fit the DSM-IV criteria for anorexia nervosa.
To quote Dr. Bulik again,
In view of the generally poor outcomes of anorexia nervosa trials, we might feel encouraged by these findings. From the outside looking in, we have to do better.
THE GOOD (AND THE BAD)
Perhaps the most important finding from this study is that, at least as far as the weight component is concerned: there were no real differences between the two manual-based approaches and treatment as usual. (The authors, by the way, predicted otherwise.) These findings mirror those found in a smaller, single-centre study in New Zealand (McIntosh et al., 2005).
While this might sound bad (If you are on a hunt for a panacea), when it comes to treating anorexia nervosa in the clinic, this is a good thing. Why? Because, as Dr. Bulik points out in her commentary, it is not feasible to train every clinician to deliver specialized treatments, and many patients might (indeed, do) live far from places where they can receive specialized therapy.
In the New Zealand study, specialist supportive clinical management—designed to be a control arm—outperformed both cognitive behaviour therapy and interpersonal therapy in the short term, and in the ANTOP study, outcomes with optimised treatment as usual did not differ significantly from the two specialised treatments. Linking family doctors to clinicians skilled in the treatment of eating disorders and guiding them through the delivery of anorexia nervosa treatment while implementing solid principles of clinical management could be an approach worth considering.
The bad, of course, is the reality that, for example, 31-41% of the patients that completed treatment had BMI’s <17.5 at 12-month follow-up. If you were to assume that everyone who had dropped out and wasn’t followed-up at the 12-month point also had BMI’s <17.5, then the number jumps even higher, to around 50%. Although this isn’t a fair assumption in part because no everyone who started treatment had BMI’s of <17.5, it is still a sobering fact.
We need to do better.
Although the findings of the ANTOP study suggest that adults with anorexia nervosa have a realistic chance of recovery or, at least, can achieve substantial improvement, a relevant proportion of patients still had anorexic symptoms at the end of our study.
In her commentary, Dr. Bulik writes, “We need to discover how to provide better, faster, and lasting results in the management of this disorder.”
I agree, but I would add something else.
Besides “discovering” better treatment options, we can do something that, in some ways is much easier, as it is clear what needs to be done, and in many ways, much, much harder. We need make treatment accessible, because right now — with many individuals waiting for months or years to get appropriate care, or fighting with their insurance companies to get coverage, or feeling the need to get sicker just to prove they need inpatient or residential help — we are not doing a good job. At all.
It is not just about discovering the optimal treatment approaches or combinations. To me, the more pressing concern is the one that’s centred around getting rid of (or at least minimizing) the social, financial, and systemic barriers that individuals face in getting treatment period.
For those on 2 year waiting lists, battling with their insurance companies, or trying to find a doctor who will diagnose them, for those trying to find a hospital that has an inpatient bed or a dietician that is within an hour’s drive, I bet the talk of treatment specifics (enhanced CBT or FPT? DBT or ACT?) sounds like a luxury few can afford.
That’s what I think needs to change first and foremost.
References
Bulik CM (2013). The challenges of treating anorexia nervosa. Lancet PMID: 24131860
Zipfel S, Wild B, Groß G, Friederich HC, Teufel M, Schellberg D, Giel KE, de Zwaan M, Dinkel A, Herpertz S, Burgmer M, Löwe B, Tagay S, von Wietersheim J, Zeeck A, Schade-Brittinger C, Schauenburg H, Herzog W, & on behalf of the ANTOP study group (2013). Focal psychodynamic therapy, cognitive behaviour therapy, and optimised treatment as usual in outpatients with anorexia nervosa (ANTOP study): randomised controlled trial. Lancet PMID: 24131861
Beautiful, empassioned account of good science. I don’t think I have anything to add, but a desire to do something political.
Wow, Tetyana. You are on a roll!!
1. I was equally thrilled by their design. The fact that they had equal groups IS AMAZING! Plus, it’s an RCT. THAT MAKES THIS STUDY EVEN MORE EXCITING! Also, I see that you bolded “ten universities in Germany” — I read that cross-institution AN RCTs are probably the most ideal given the low prevalence rates of the disorder.
2. Loved that the 60% of the sample consisted of patients who had been struggling with their ED for 6 years or less. Seems like a more accurate representation of the majority of patients.
3. Yep, those unfamiliar with AN trials may think that 30% is too high a dropout rate but honestly that % already trumps other trials in the literature!
4. I absolutely agree re: your point about accessible and affordable treatment, especially when we consider the fact that the longer sufferers have to wait, the longer they may/will remain ill. And as you know, the longer the illness duration, the poorer the outcome.
5. The results of this study are not ideal, like you and Dr. Bulik have already pointed out. I’m hoping that future studies will build on this study, i.e. replicate the strengths and improve on the limitations.
What an interesting article. I’m a therapist who treats EDs and AN is particularly difficult to treat. As you said though, most of the time it’s just as difficult to get over treatment barriers, like insurance or availability. Keep at it though! We definitely need “better, faster, and longer lasting treatments.”
Absolutely, patients need access to treatment . . . but, it is imperative that it is being provided by qualified professionals using the best treatment approaches possible. One of the significant hurdles we discovered over an eight year (and counting) battle with ED for a family member was finding qualified therapists with the necessary training and clinical experience. Many therapists advertise this as an area of focus . . . far fewer actually have the skills.
Make no mistake, discrimination by insurers against those with serious mental health conditions is rampant. However, having spent over $650,000 including insurer coverage over a four year period for the treatment of a daughter, the issue is not just insurers. We could write a book on this subject.
Hi James,
I completely agree: We do need more qualified professionals, absolutely. That requires better training, and of course everyone has their own idea on what that entails/should entail, myself included. Research shows many clinicians and nurses actually want more training in this area, too.
Tetyana