As of January 2014, over 50% of adults in the United States own a smartphone; unsurprisingly, there has been a growth in the number of mobile applications (apps) aimed at providing health care services for various mental (and physical) health problems, including eating disorders. The purpose of mobile health technologies is to utilize the functionality of smartphones to deliver a wide range of health services, including providing psychoeducation, treatment services and/or recovery support.
POTENTIAL BENEFITS OF SMARTPHONE APPS FOR ED TREATMENT
When it comes to the treatment of EDs, there are many potential benefits of smartphone apps. Smartphone apps can potentially help increase access to treatment (if, for example, they link users to ED services), enhance treatment compliance and/or engagement, and support treatment “outside of the therapy office.” Apps may also be able to improve motivation by connecting individuals to others who are recovering from EDs.
Smartphone apps can increase access to treatment since they provide a cheaper (often free) alternative to in-person meetings and transcend geographical barriers. They can also provide customized support in real-time. Finally, they may be preferred by individuals who feel ambivalent about seeking treatment or who feel a lot of stigma and shame about their ED.
Of course, while it is unlikely that apps will be sufficient to replace face-to-face treatment (at least in most cases), they could help improve symptoms and generally facilitate treatment/recovery. However, the potential utility of these apps is at least partially related to their utilization of evidence-based treatments/principles (EBPs).
ED TREATMENT APPS AND EVIDENCE-BASED PRINCIPLES
So, how do existing ED treatment apps measure up? Do they utilize empirically-based principles? And to what extent do they utilize advanced in smartphone technology? These are the primary questions that Adrienne Juarascio and colleagues sought to answer in their recent paper published in the European Eating Disorders Review.
The authors identified six apps that were specifically “treatment-focused”: Recovery Record, RiseUp: Overcoming Your Eating Disorder, Before I Eat, iCounselor: Eating Disorder, Stop Binge Eating: Lose Weight, and Daytime Affirmations.
To be completely transparent: I have not used any of these apps, although I’ve been introduced to the RiseUp app by its creator, Jessica Raymond, and I may have downloaded and flipped through the Recovery Record app at some point (but I cannot recall clearly). I have never heard of the other apps reviewed.
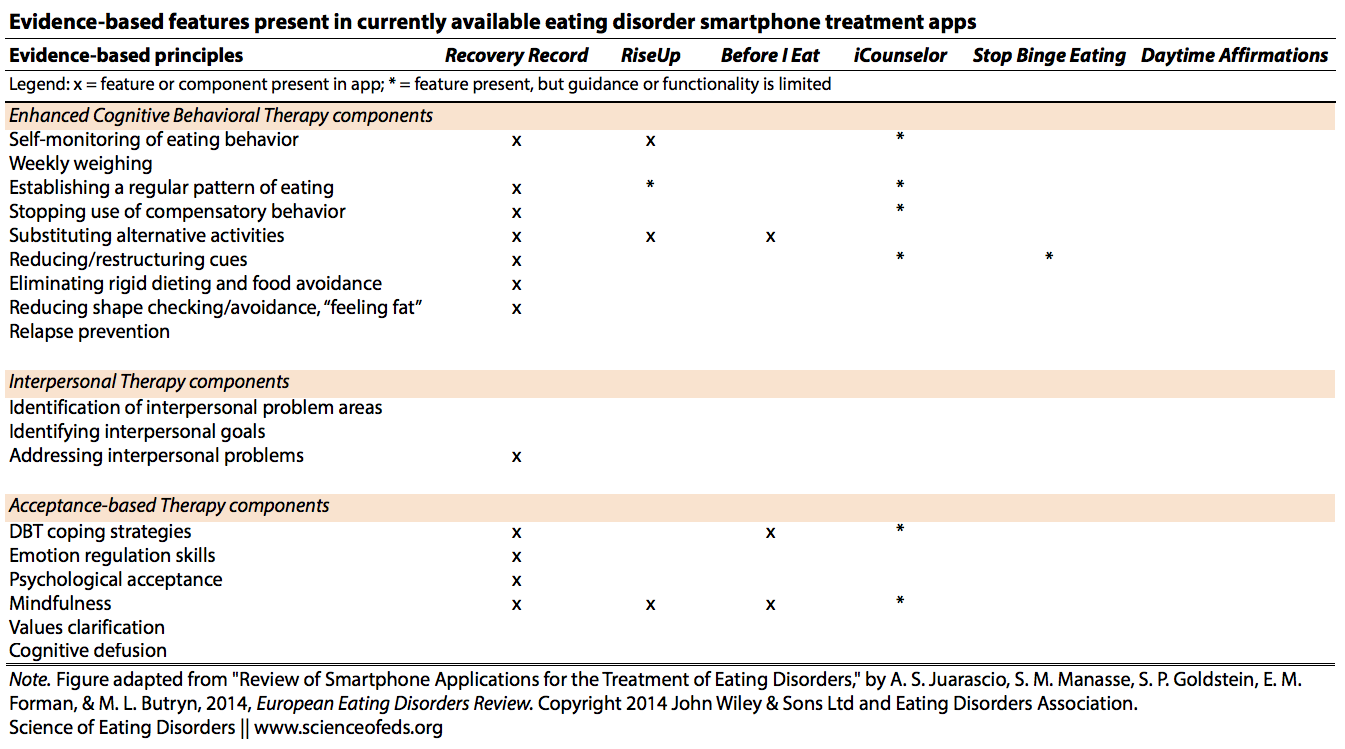
First, the authors assessed whether the apps utilized EBPs. More specifically, they assessed whether the apps contained components of (enhanced) cognitive behavioral therapy (CBT/CBT-E) and interpersonal therapy (IPT), both of which are considered effective treatment for adults with EDs. They also reviewed for components of acceptance-based therapy (ACT, which the authors write “are beginning to show empirical support for treating EDs.”) They also examined the apps for information on nutritional management, but found that none of the apps they assessed had this component.
SUMMARY OF MAIN FINDINGS
Here’s a summary of what they found (click on the image to enlarge):
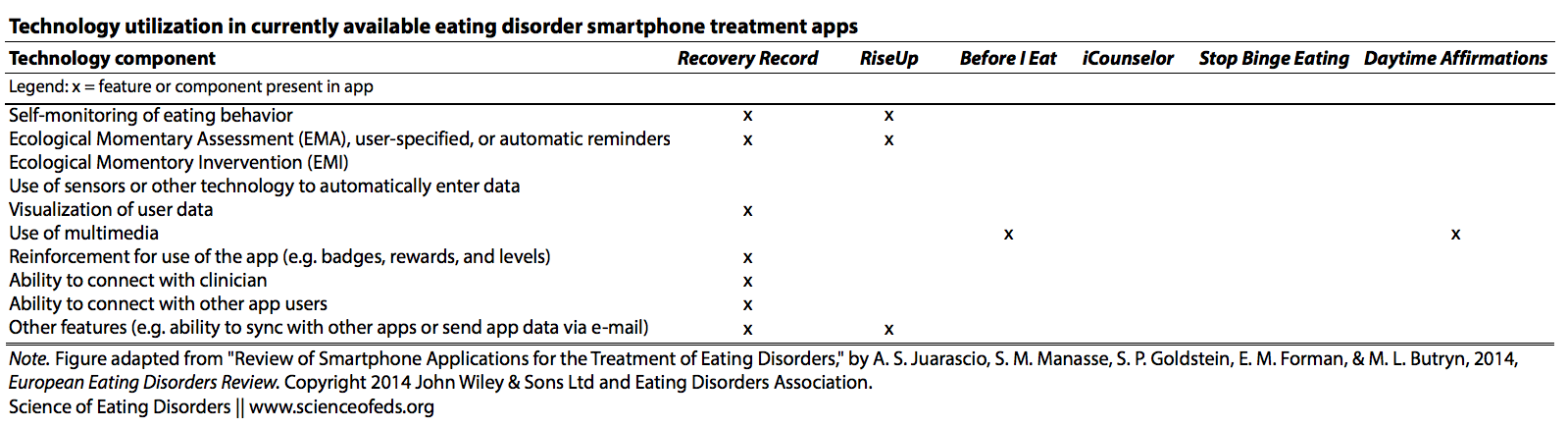
This is a summary of what the authors found when they assessed the apps’ utilization of smartphone technology:
Clearly, both with respect to EBPs and technology utilization, Recovery Record is far above the rest. Juarascio et al. note that Recovery Record contains a wide range of features, including “self- monitoring, personalized coping strategies, social connection, and a portal to connect with the user’s clinician.”
According to Juarascio et al.’s analysis, both RiseUp and iCounselor contain some EBP components, but much of the content is not empirically-supported. Stop Binge Eating and Daytime Affirmations are particularly weak with regard to including empirically-supported interventions, and, along with iCounselor and Before I Eat, in utilizing smartphone technology.
The authors conclude,
Although it would be impossible (and likely ineffective) for any app to include all of the empirically support treatment components we assessed for, most apps reviewed in this study contained few if any evidence-based principles. Additionally, many of the apps reviewed contained primarily non-empirically supported treatments. For example, Daytime Affirmations solely offers guided imagery. Stop Binge Eating offers coping strategies that are inconsistent with empirically supported treatments for binge eating such as ‘eat something healthy.’
POTENTIAL RISKS OF SMARTPHONE APPS
I mentioned some benefits of using smartphone apps to assist with ED treatment, but there are important risks that must be considered, particularly given the generally low level of EBP utilization across the apps reviewed. Juarascio et al. mention that the availability of these apps may lead people to avoid seeking in-person professional treatment (even when it is “available and warranted”).
There is also potential for the apps to interfere with treatment in cases where the apps may provide conflicting information or information that contradicts a treatment provider’s recommendations. Of course, advice and feedback from others using the app may be unhelpful and/or harmful. While neither of these are unique to mobile apps (there’s plenty of harmful or unhelpful advice on online forums, and, frankly, from treatment providers), I think there’s a danger when the unhelpful or even harmful advice comes from sources that appear to be “legitimate.”
As Juarascio et al. alluded to in the aforementioned quote, I think apps may provide individuals with a facade that they are utilizing EBPs when that may not be the case. The damage here, of course, is that the so-called “coping strategies” may actually do harm to the person:
Although the non-empirically supported components included in these apps are not necessarily ineffective or iatrogenic, it may be particularly important to view these components with more caution as there is minimal or no data to support their inclusion.
Those writing on e-therapy, I think Christina Loucas and colleagues‘ concerns are applicable here, too:
For example, people with eating disorders (and those around them) may think that by using an app they are addressing their eating disorder whereas in reality they may be simply delaying their entry into an empirically-supported form of treatment.
FUTURE DIRECTIONS
The authors provide several suggestions for future app developers/development, including (but not limited to):
- in-the-moment/automatically-delivered interventions drawn from EBTs that the patient reported to be the most helpful,
- feedback based on information entered by the user,
- messages based on pre-intervention behavior patterns
Future apps could also incorporate “programmed machine learning,” providing customized feedback based on identified automatically detected) “high-risk situations” and “personalized feedback on treatment progress on both assigned goals/homework and self- monitoring records.” The authors also call for more customizable apps that allow users to, for example, “save particular strategies that are most effective.”
CONCLUSION
Juariscio et al.’s group is developing their own app (TakeControl) that seeks to address some of the limitations of currently available apps. Given this, I think it is important to take the paper’s critiques with a grain of salt–it is not that they are not valid, but I do think they are probably framed in a particular way (i.e., likely focusing more on limitations that TakeControl aims to directly address and perhaps ignoring other limitations that TakeControl might also have). I think it might be fair to consider the fact that the authors’ are developing their own app as a conflict of interest, but maybe not.
I also think it is important to point out the distinction between treatments (or app components) where there is not a sufficient evidence base regarding whether they work and those where there is sufficient evidence that they do not work. There’s a difference between including components that haven’t been tested empirically and including those that have been tested and have been shown to not work.
As Juarascio et al.’s paper was quite long, this post reflects and summarizes only a small portion of what was discussed. Feel free to raise any relevant point in the comments, even if they were not directly addressed in the post.
I’m very curious to hear from individuals who have used these apps. How did you find them? And what do you think about the call for utilizing more EBPs in ED treatment apps?
References
Juarascio, A.S., Manasse, S.M., Goldstein, S.P., Forman, E.M., & Butryn, M.L. (2014). Review of Smartphone Applications for the Treatment of Eating Disorders. European Eating Disorders Review PMID: 25303148
I tried a few but never liked any of them. I don’t remember what I tried but remember it being a combination of CBT strategies, affirmations, and manual meal logging without the calorie counts.
I personally found them condescending and unhelpful. I can’t stand affirmations and CBT has never worked with me… I also dislike having a log of my meals as it’s triggering.
I had a therapist who requested that I text her meal logs as I ate and provided no commentary until I saw her again at my next session (if any commentary at all). It was for her knowledge and allowed me to stop fixating and just send out the info without tracking it. I could delete the message convo if I wanted so I didn’t have to have any record while knowing that it was still being monitored.
Hey Lauren,
Thanks for the comment! I’m curious, what did you find condescending about them? I suspect I’d feel the same way if I were to use them for any prolonged period of time. I personally really dislike affirmations and any positive/”motivational” quotes; they put me off so much. I really can’t stand them.
I can see how entering the meals would be triggering. Flipping through RiseUp and Recovery Record, I found it too cumbersome. I also would much prefer to enter calories as opposed to specific foods. It is just my preference, and it is what has worked for me in the past when I was working on normalizing my intake.
In the end, when I did track my intake or mood (or anything else, for that matter), I used excel. I find it gives me the most flexibility and it also enables me to analyze the data in any way I want, which I find super helpful. The downside, of course, is that it is desktop-based and I can’t have random alerts on my phone.
The only app I’ve liked is a mood tracking app called Mood. It is super simple. I like it not because I track the data so much, but because the multiple-times-a-day prompts to enter my mood and energy levels alerts me to be mindful of my mental state. I don’t think it is made much of a difference in anything though, but it is just two questions I need to fill out, so it is not a hassle. Optimism is also good, but I never used it for long enough.
I found the same aspects that you dislike about affirmations condescending. I’m more open to things like meditation right now, but when I was borderline suicidal and/or dealing heavily with my eating disorder I would get incredibly angry when being taught that affirmations or guided meditation would resolve my issues.
Yeah, I can imagine; I find those things are particularly annoying when in a particularly difficult (err negative?) state. I tend to just find them useless. I often find those motivational quotes or affirmations annoying also because they often sound like they are coming from a tremendous place of privilege, but that might just be my negative interpretation.
Hi Tetyana, this post is super timely for me – we are working on a guide for school guidance teachers and in the most recent round of feedback we were asked to identify good apps staff could recommend to students.
I share your concerns with an app substituting for professional treatment…..but then with a younger age group not sure about the level of risk. Your thoughts?
Looking forward to reading more comments.
Hi Shaleen,
I’m a bit confused: Who are the students that the apps you/the teachers are looking for would be recommended to? Individuals with eating disorders? I think for individuals without eating disorders, or for those in the earlier stages of the ED/disordered eating, these types of apps (depending on the app *AND* on the symptoms) can do more harm than good.
Tetyana
Hey! I spent quite a bit of time playing around with Recovery Record for a mobile app course I was in. A few features that struck me were level of detail for recording meals (I also think that this would be triggering for me by forcing me to dwell on my intake) and the very feminine user interface and affirmations (sexist?). I also wish there was an automatic record of location built in, which would be quite easy with many of the GPS APIs currently available. I think there was a mood component, but no feedback on how mood correlates with eating behavior, which would be helpful in my opinion.
I can try and see if I still have my notes on the RR app from my class records if you need them. I think the app is free still? I don’t know much about the other apps.
Hey,
Yeah, from what I remember, the level of detail was kind of cumbersome for me (but that’s just me). Good point on the feminine user interface! I never really thought about that, but that’s very very true. I agree with the mood stuff — correlating mood with behaviour is what I always wanted from an ideal app (but in EMA style, not in recording it once or twice a day or something). I think the Optimism app would allow you to correlate mood with behaviour, but I am not 100% sure on that.
Re automatic stuff, Juarascio made a lot of points on this, too. They also mention automatic recording of location, for example: “Furthermore, the capabilities of app sensors (e.g. GPS) allow for the automatic recording of information to reduce user-burden” and “Overall, app functionality in ED intervention apps appears to be very limited. No app supplemented manual data entry with automated data entry (e.g. geolocation, time). Additionally, none of the apps featured personalized EMIs or automatically-delivered EMIs during identified times of high risk.”